MEDICAL NEWS

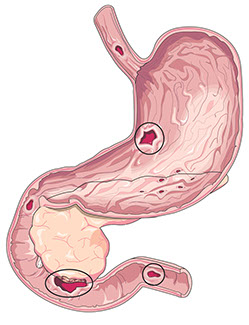
The lining of your stomach makes acid and enzymes that help break down food into the nutrients you need. The lining protects itself from acid damage by releasing mucus. But sometimes the lining gets inflamed and starts making less acid, enzymes, and mucus. This type of inflammation is called gastritis.
You may have gastritis if you have pain or an uncomfortable feeling in your upper stomach. You could have nausea or vomiting. Or you may have no symptoms at all.
Untreated, some types of gastritis can lead to ulcers. These are sores in the stomach lining.
Some people think ulcers are caused by stress and spicy foods. But according to the NIH in Health, bacteria called H. pylori are often to blame. These bacteria break down the inner protective coating in the stomach and can cause inflammation.
H. pylori can spread by passing from person to person or through contaminated food or water. Infections can be treated with antibiotics.
One type of gastritis, called erosive gastritis, wears away the stomach lining. The most common cause of erosive gastritis is long-term use of medications called non-steroidal anti-inflammatory drugs. These include aspirin and ibuprofen. Stop taking these pain relievers and the gastritis usually clears up.
Less common causes of gastritis include digestive disorders (such as Crohn’s disease) and autoimmune disorders in which the body’s protective immune cells attack healthy cells in the stomach lining.
Gastritis can be diagnosed with an endoscope. A thin tube with a tiny camera on the end is inserted through the patient’s mouth or nose and into the stomach. The doctor looks at the stomach lining and may remove some tissue samples for testing. Treatment will depend on the type of gastritis found.
Although stress and spicy foods don’t cause gastritis and ulcers, they can make symptoms worse. Milk might provide brief relief, but it also increases stomach acid, which can worsen symptoms. Your doctor may advise taking antacids or other drugs to reduce acid in the stomach.
Gastritis can lead to ulcers over time. Symptoms of ulcers include pain between the belly button and breastbone that starts between meals or during the night. It briefly stops if you eat or take antacids, lasts for minutes to hours, and comes and goes for several days or weeks.
Contact your doctor right away if you have sudden sharp stomach pain that doesn’t go away, black or bloody stools, or vomit that is bloody or looks like coffee grounds.