Dental problems affect more than your teeth and mouth. Gum (periodontal) disease and other mouth infections may increase the risk for:
* Pneumonia.
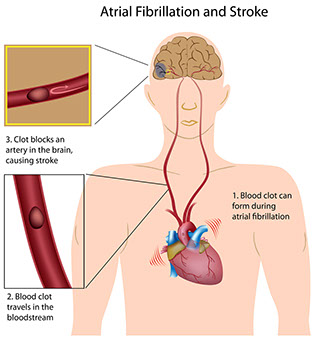
* Heart disease.
* Diabetes.
Also, an oral exam can help a dentist detect many health problems. These include diabetes, eating disorders, heart disease, osteoporosis, and a lack of vitamins.
Brush Your Teeth
* Do this twice a day. Brush more often, if you need to.
* Use a soft-bristled toothbrush and a toothpaste with fluoride. Brush with a gentle touch. If you have sensitive teeth, use a toothpaste made for this.
* Do a thorough job. Brush in small circles across all of the surfaces of the upper and lower teeth. Brush the outer, inner, and chewing surfaces. Brush the surfaces between the teeth.
* A child younger than 7 years old and some handicapped persons may need help to do a thorough job. A mechanical tooth brush may be helpful.
* Use a toothbrush that fits your mouth. Change your toothbrush to a new one every 3 to 4 months. Do this more often if the bristles are bent or frayed. Change it after having a throat or mouth infection, too.
* Brush your gums gently. Keep the brush perpendicular to your teeth.
* Gently brush your tongue. It can trap germs.
Floss Your Teeth
* Floss or use an interdental cleaner once a day to remove food particles and plaque from areas that your toothbrush cannot reach.
* Use a piece of floss about 1-1/2 feet long.
* To floss your upper teeth, hold the floss tightly between the thumb on one hand and index finger on the other. Using a gentle, sawing motion, bring the floss through the tight spaces between the teeth. Do not snap it against the gums.
* With the floss at the gum line, curve it into a C-shape against one tooth and gently scrape the side of it with the floss. Repeat on each tooth. Use a fresh section of floss for each tooth.
* Repeat for your lower teeth, but hold the floss between both index fingers.
* Rinse your mouth after flossing.
* If it is hard for you to use dental floss, use a dental floss holder sold in drugstores.
* After flossing, rinse your mouth with water, mouthwash, or an anti-microbial mouthrinse.
It is normal for gums to be tender and bleed for the first week. If the bleeding continues, see your dentist.
More Tips
* Protect your teeth from damage and injury.
* Ask your dentist if you should use a fluoride mouth rinse, a prescribed toothpaste with fluoride, fluoride supplements, and/or a water-pik device.
* Don’t lay a baby down with a bottle left in the baby’s mouth if the bottle contains juice, milk, soda, etc. Water is okay, though.
Get Regular Dental Checkups
See your dentist every 6 months, at least every year, or as often as your dentist advises. Regular dental checkups are important to:
* Clean your teeth and remove plaque and tarter that buildup even after you brush and floss every day. Removing plaque and tartar helps prevent cavities, gum disease, and other problems.
* Check for cavities, gum disease, oral cancers, tooth grinding, bite problems, and other problems. When these are detected early, they are easier to treat.
* Address any areas of concern.
* Find out how to take care of your teeth and what dental care products you should use.
Also, an oral exam can help a dentist detect other health problems, such as diabetes, heart disease, eating disorders, and osteoporosis.
Diet & Dental Health Tips
* If your local water supply has fluoride, drink 6 to 10 cups of tap water every day. If not, make sure to use a fluoride toothpaste.
* Eat a well balanced diet. Limit between-meal snacks.
* Eat sticky, chewy, sugary foods with (not between) meals. Finish a meal with foods that help buffer acid formation. Examples are cheese, meat, fish, nuts, and dill pickles.
* Avoid sugar-sweetened gum and beverages. Chew a sugar-free gum instead, especially one with the artificial sweetener xylitol.
* Don’t eat sweets, fruit, or starchy foods just before bedtime. Your mouth makes less saliva during the night. This allows cavity-causing bacteria to feed on food particles. Brushing your teeth doesn’t effectively prevent this.