Brain & Nervous System
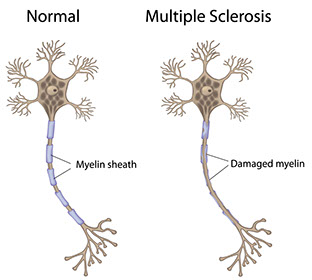
Multiple Sclerosis (MS) is a chronic disease of the brain and spinal cord. With MS, a covering that protects nerves (myelin) and the nerves are damaged or destroyed. Over time, scar tissue forms along the damaged myelin. Nerves can’t send signals like they should. As a result, movement, sensation, etc. are impaired or lost.
Signs & Symptoms
* Fatigue.
* Feelings of pins and needles. Numbness. Leg stiffness.
* Poor coordination. Unsteady gait. Impaired movement.
* Bladder problems.
* Blurred vision. Double vision. Loss of vision in one eye.
* Depression. Mild problems with memory, learning, etc.
* Swallowing problems.
Early signs and symptoms may be mild and present for years before MS is diagnosed.
Symptoms vary from person to person. They may last for hours or weeks. They can vary from day to day and can come and go with no set pattern.
Some persons have only a few symptoms over the course of the disease. For others, symptoms continue and/or worsen with time. Most persons with MS get symptom flare-ups (relapses) that are followed by partial or complete recoveries (remissions).
Causes
The exact cause of MS is not known. It may be due to a number of factors. These include: A virus, genetics, and an immune system problem. Toxins, trauma, poor nutrition, and other factors may also play a role. Things known to come before the onset of MS include: Overwork; fatigue, the postpartum period for women; acute infections; and fevers. Multiple sclerosis is more common in:
* Women than in men.
* Caucasians than in Hispanics or African Americans. It is rare among Asians and certain other ethnic groups.
* Adults between the ages of 20 and 50. Young children, teens, and older adults can also have MS.
* People who are born and live up to at least age 15 years old in places farther from the equator. These include North America, Europe, and Southern Australia.
Treatment
There is no cure yet for MS, but most people with it live a normal life span. Treatment for MS includes:
* Prescribed medication to lessen the number and severity of flare-ups and to slow the progression of the disease. Research favors early treatment with this type of medicine.
* Short-term courses of IV or oral corticosteroids. These reduce inflammation during MS flare-ups.
* Medications to control and treat MS symptoms. Treating infections, when present.
* Physical and occupational therapy.
* Counseling. Support groups.
* Clinical trails. Accesswww.clinicaltrials.gov.
Questions to Ask
Self-Care / Prevention
* Follow your doctor’s guidelines for home care.
* Maintain a normal routine at work and at home. Avoid activities that lead to fatigue or put too much physical stress on the body. Get plenty of rest.
* Manage emotional stress.
* Avoid the heat and sun. Don’t take hot showers or baths. Increased body temperature can cause symptoms. Cool baths or swimming in a pool may improve symptoms by lowering body temperature.
* Have body massages to help maintain muscle tone.
* Treat a fever as soon as it occurs.
* Get regular exercise. Physical therapy may be helpful.
* Get counseling, if needed.
* Get a seasonal flu shot every year and other vaccines as advised.
* If you smoke, quit!
Resources
Multiple Sclerosis Foundation
888.MS.FOCUS (673.6287)
National Multiple Sclerosis Society
800.FIGHT.MS (344.4867)www.nationalmssociety.org














