MEDICAL NEWS

Your A1C number is one of the most common markers your doctor may use to check for or monitor your blood sugar. For someone with diabetes or prediabetes, A1C is a crucial tool to assess your blood sugar management over time.
Compared to blood glucose levels which measure how much sugar is in your blood at that exact moment, A1C gives a snapshot of your average blood glucose levels over about three months.
What does A1C measure?
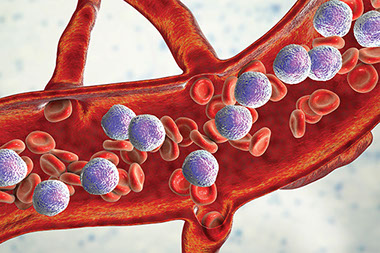
A1C measures the percentage of red blood cells (or hemoglobin) in your blood that have glucose attached to them.
It is normal for hemoglobin to pick up some glucose from the bloodstream. However, someone who has prediabetes or diabetes has too much glucose in their bloodstream. As a result, a higher percentage of hemoglobin in the blood will end up holding sugar.
Because the lifespan of a hemoglobin cell is about 3-4 months, the A1C test can give a big picture look at your blood glucose control over time.
What is an ideal A1C?
In general, A1C levels fall into three categories:
* Normal: Under 5.7%
* Prediabetes: Between 5.7% and 6.4%
* Diabetes: Over 6.5%
When it comes to an “ideal” A1C, that depends on your individual situation and the goals you set with your doctor. For people with diabetes, a common goal is for A1C to be below 7%. Talk to your doctor to find out your ideal A1C.
Factors that influence A1C
Anything that affects your blood glucose levels will impact your A1C. The most common factors include:
* Body weight – overweight or obesity interferes with blood sugar control.
* Nutrition – a poor diet can impair blood sugar regulation.
* Movement – a sedentary lifestyle increases your risk of prediabetes and diabetes.
* Iron deficiency anemia – can result in a falsely high A1C due to low total hemoglobin.
* Illness or stress – glucose levels are naturally high when physically or mentally stressed.
Can I reduce my A1C?
Yes. If your doctor tells you your A1C is high, they may recommend lifestyle changes to improve your blood glucose control.
* Exercise: Getting a minimum of 150 minutes of moderate to vigorous activity each week can improve your glycemic control.
* Weight loss: Studies have shown that losing 5% to 10% of body weight may modestly lower A1C.
* Eating a healthy diet: A mostly plant-based diet that is low in processed and junk foods is a good option for weight management and glycemic control.